
The surprising way high blood pressure can change your skin as you get older
The Surprising Way High Blood Pressure Can Change Your Skin as You Get Older
Many individuals with high blood pressure are aware of its risks to heart health and the increased likelihood of strokes. However, there’s another consequence of chronic hypertension that often goes unnoticed: its effect on the skin. As we age, the skin naturally becomes thinner and more fragile, but high blood pressure can accelerate this process, making the skin even more vulnerable. Let’s explore how high blood pressure silently damages the skin, particularly in older adults, and what you can do to protect both your skin and your overall health.
Key Takeaways:
-
Chronic high blood pressure increases skin fragility, making it more susceptible to tears, bruises, infections, and slow healing.
-
The fragility is a result of small blood vessel damage and the thinning of the skin caused by both aging and hypertension.
-
Skin injuries are not just cosmetic; they can lead to serious complications and reduced independence.
-
Managing blood pressure and protecting your skin can help preserve both your appearance and health.
1. The Domino Effect: How High Blood Pressure and Age Weaken Your Skin
As you get older, your skin naturally loses some of its strength, particularly in the dermis (the supportive layer), which thins and loses collagen and elastin. When combined with years of living with high blood pressure, this thinning skin becomes even more fragile. Hypertension exerts constant pressure on the tiny blood vessels, or capillaries, in your skin. The result? Your skin becomes prone to tearing and bruising with minimal trauma, such as minor bumps or pressure.
2. Common Signs of Fragile Skin
Older adults with hypertension often notice that their skin bruises or tears from even small bumps or pressure that wouldn’t have caused any issues previously. Minor injuries that once went unnoticed may now lead to visible bruises (often called senile purpura) or even tears. Skin can become more easily torn by adhesive bandages, and injuries may take much longer to heal than they would in younger, healthier skin.
3. Why Fragile Skin Leads to Bigger Problems
Skin injuries aren’t just superficial—they can quickly escalate into more serious problems. Hypertension reduces blood flow, which in turn slows down the body’s ability to heal wounds. A tear in fragile skin is also an entry point for bacteria, leading to infections and potentially serious complications. Studies show that skin tears are prevalent in older adults, with a prevalence of up to 11% annually, and they’re even more common in nursing homes (Strazzieri-Pulido et al., 2015).
4. The Cycle of Slow Healing and Recurrent Wounds
Impaired circulation, coupled with weakened skin, can cause every minor bump or scrape to become a recurring issue. As each new wound heals, it may leave behind scarring, making the skin stiffer and more prone to future tears. Over time, this cycle increases the risk of chronic sores, particularly on the legs, which can be painful and difficult to treat.
5. Bruising and Vascular Marks: More Than Cosmetic Issues
Unexplained bruising is common in people with fragile skin. The capillaries under the skin rupture easily, causing visible bruises. These bruises can be concerning because they may resemble signs of serious illnesses or mask underlying conditions. In addition, visible veins and broken blood vessels are indicators of vascular weakness, signaling that the skin is vulnerable and may be prone to more serious injuries.
6. Infection Risks Increase
With the skin’s protective barrier compromised, it becomes an open gateway for infections. Older adults, who may already have a slower immune response, are particularly at risk for infections such as cellulitis. Chronic wounds can harbor harmful bacteria or fungi, leading to serious infections that may require hospitalization or long-term care (LeBlanc et al., 2013).
7. Other Skin Conditions Become Harder to Control
In addition to becoming fragile, aging skin tends to become dry, itchy, and more sensitive. High blood pressure contributes to this by damaging tiny blood vessels, reducing circulation. This creates an environment that makes chronic skin conditions such as eczema or stasis dermatitis more likely to flare up, and harder to manage effectively.
8. Leg Swelling: Edema Makes Things Worse
Hypertension and the medications used to treat it can contribute to swelling in the legs and ankles, a condition known as edema. This swelling stretches the already fragile skin, making it more susceptible to cracks, ulcers, and pressure sores. These wounds are particularly difficult to heal and can further reduce mobility and quality of life.
9. Loss of Mobility and Independence
Pain from skin injuries or the fear of further skin tears often causes older adults to limit their movements, leading to reduced activity. This decreased movement results in worsened circulation, diminished muscle tone, and further deterioration of skin health. This cycle can significantly affect mobility and independence, making it harder to live a full, active life.
10. Increased Healthcare Needs and Costs
Fragile skin increases the need for medical attention. Every wound or infection may require trips to the doctor or hospitalization, raising healthcare costs and extending treatment times. In long-term care facilities, managing skin tears and pressure sores is one of the most resource-intensive tasks (Falanga, 2005).
11. Prevention: What You Can Do
-
Control your blood pressure: Follow your doctor’s advice, including medication, a balanced diet, and regular exercise.
-
Protect your skin: Wear long sleeves, use protective padding when necessary, and be gentle when cleaning or handling your skin.
-
Moisturize regularly: Use fragrance-free moisturizers to keep your skin hydrated and less prone to cracking.
-
Practice careful wound care: Even small cuts require immediate attention. Keep them clean, covered, and watch for signs of infection.
-
Address swelling: Elevate your legs when resting and use compression as recommended by your provider. Report any sudden or severe swelling immediately.
-
Nutrition matters: A diet rich in vitamins C and E, protein, and healthy fats supports skin health and repair.
-
Move regularly: Gentle activity, such as walking, stretching, and light resistance training, can help improve circulation and skin strength.
Conclusion
High blood pressure is a silent contributor to skin damage, especially as you age. By understanding how hypertension impacts skin health, you can spot the warning signs early and take proactive steps to protect yourself. Keeping your blood pressure under control, moisturizing your skin, and managing circulation can help preserve the health of your skin and maintain your independence for years to come.
Sources:
-
Centers for Disease Control and Prevention (CDC), Hypertension Prevalence Among Adults Aged 60 and Over: CDC Website
-
Strazzieri-Pulido KC, Peres GR, Campanili TCGF, Santos VLCG. Incidence of skin tears and risk factors in a nursing home. J Wound Ostomy Continence Nurs. 2015;42(3):235-239. doi:10.1097/WON.0000000000000125
-
LeBlanc K, Baranoski S, Christensen D, et al. International Skin Tear Advisory Panel: a tool to classify skin tears. Adv Skin Wound Care. 2013;26(11):519-524. doi:10.1097/01.ASW.0000435937.65008.9e
-
American Academy of Dermatology Association, Effects of high blood pressure on the skin: AAD Website
-
Falanga V. Wound healing and its impairment in the diabetic foot. Lancet. 2005 Nov 12;366(9498):1736-43. doi:10.1016/S0140-6736(05)67700-8
News in the same category


Nature’s Secret Healer: Discover the Astonishing Powers of Kyllinga Brevifolia for a Healthier You

10 supplement combos that cancel out each other’s benefits

4 things that overestimate your heart if you already have heart problems

Castor Oil After 50: This Is What Happens After 7 Days Of Use!

Unlock the Secret Benefits of Olive Oil

Nine Year Study Finally Explains The Relationship Between Sugar And Cancer

These 9 foods contain compounds that disrupt breast cancer cells

Rosemary tea: drink it for 15 days and see what happens
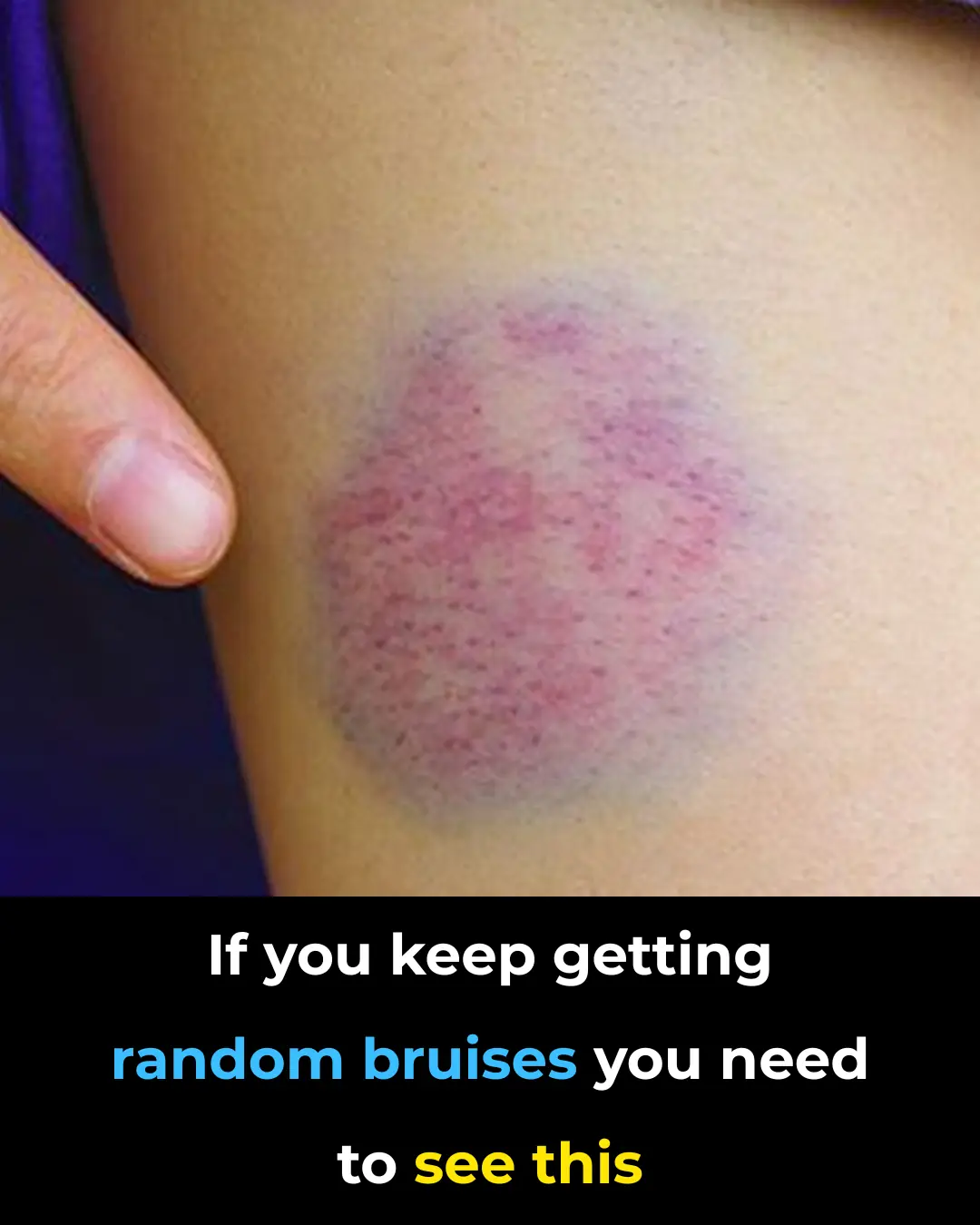
Unexplained Bruising on Your Body: Causes and Treatments

15 Nighttime Signs of Diabetes You Shouldn’t Ignore

Diabetes? Just boil these leaves to lower blood sugar (without medications)!

The Hidden Health Risks of 4 Foods You Thought Were Clean

Put THIS Mixture Under Your Tongue Before Bed And NEVER Wake Up Tired Again!

These 14 Foods Will Improve Your Kidneys’ Ability To Detox Like Never Before!
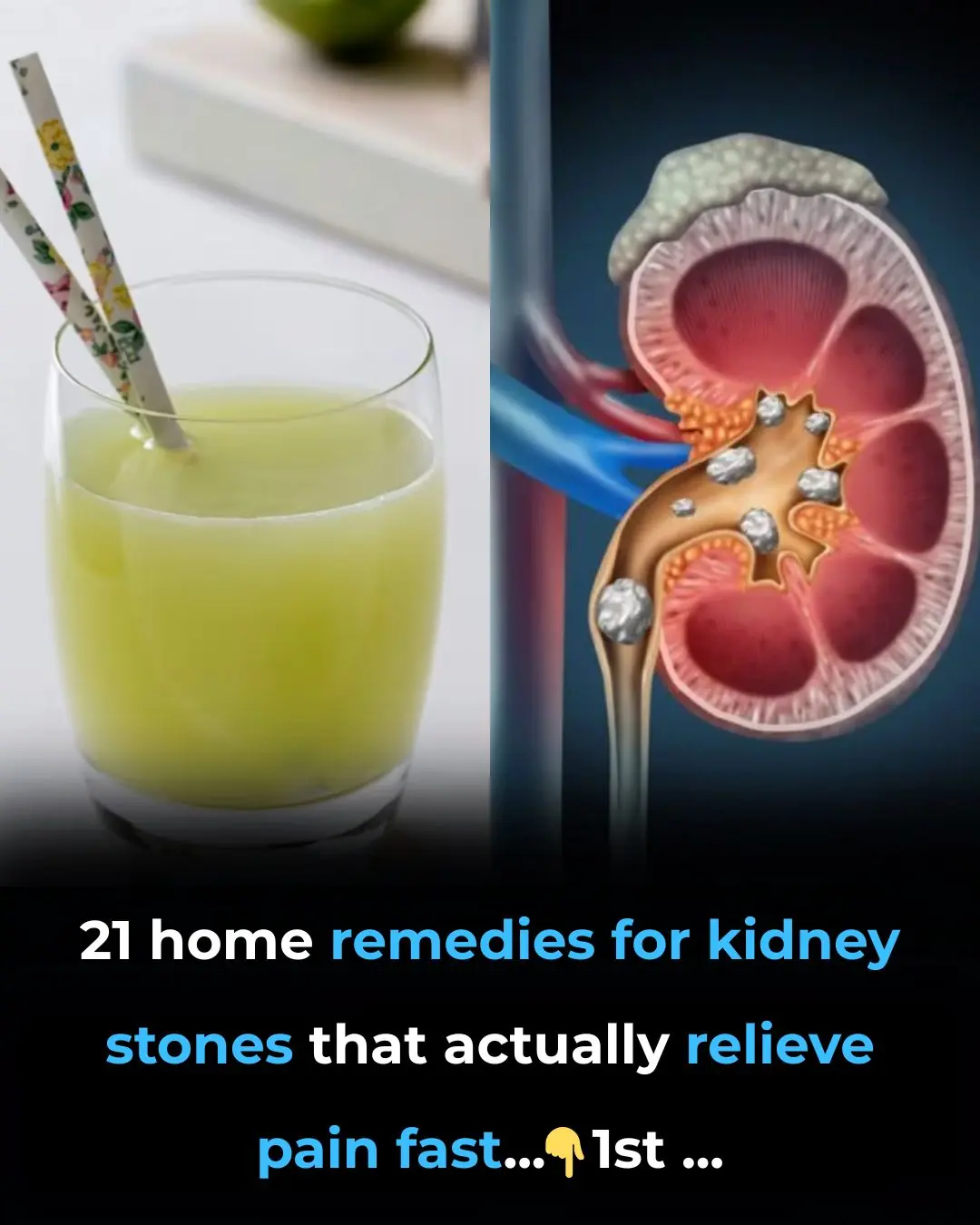
Home Remedies For Kidney Stones – 21 Remedies For Effective Pain Relief

Diabetes? Just boil these leaves to lower blood sugar (without medications)!

How to Make Homemade Clove Oil and the Powerful Benefits It Offers

9 Foods You Should Eat Regularly to Prevent Memory Loss and Keep Your Brain Sharp as You Age
News Post

Mimosa Pudica: The Gentle Plant with Powerful Wellness Benefits
Don’t Toss Those Onion Peels — They’re Nature’s Hidden Remedy

Nature’s Secret Healer: Discover the Astonishing Powers of Kyllinga Brevifolia for a Healthier You

The Plaster That Re-Grows Teeth – The Revolution That Changes Dentistry

Eat Eggs but NEVER Make These 7 Mistakes — They Can Be Dangerous for Seniors

Boil a banana with cinnamon and drink it tonight; it's much more powerful than pills!

10 supplement combos that cancel out each other’s benefits

4 things that overestimate your heart if you already have heart problems

Your Brain as a Chemical Factory: How Thoughts Shape Your Health and Well-Being

Scientists Unlock the Brain’s Potential to Restore Forgotten Memories Through Silent Neuron Reactivation

Groundbreaking Discovery Enhances Immune Cells to Fight Cancer More Aggressively

Castor Oil After 50: This Is What Happens After 7 Days Of Use!

Breakthrough Discovery Targets Dormant Cells to Prevent Breast Cancer Recurrence

Unlock the Secret Benefits of Olive Oil

Nine Year Study Finally Explains The Relationship Between Sugar And Cancer

Fungi as the Future of Data Storage: How Mushrooms Could Revolutionize Digital Systems

American Sweetgum (Liquidambar styraciflua): The Forgotten Healing Tree

Man in China Fines Officials with Coins, Making a Silent but Powerful Statement
