
When your liver is bad. Please check if this is correct.
When your liver is not functioning properly, the body often sends warning signals—but many people fail to recognize them early.
The liver is one of the most vital organs in the human body. It performs more than 500 essential functions, including detoxifying harmful substances, producing bile for digestion, regulating blood sugar, storing vitamins and minerals, and supporting immune function.
Because it plays such a central role, liver problems rarely stay isolated.
When the liver is “bad” or damaged, other parts of the body begin to hurt or show symptoms.
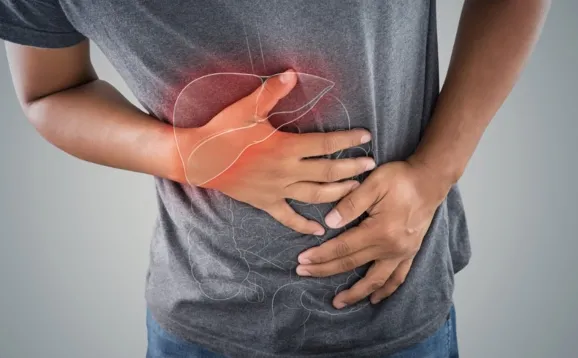
One of the first places people may feel pain is in the upper right abdomen.
The liver is located in the upper right side of the belly, just beneath the rib cage.
When it becomes inflamed due to conditions such as hepatitis, fatty liver disease, or alcohol-related damage, the liver can swell.
This swelling stretches the protective capsule around the liver, causing a dull, persistent ache or sharp discomfort in that area.
Some people describe it as pressure or fullness rather than intense pain.
This symptom is often ignored until it becomes severe.

The right shoulder and upper back can also begin to hurt.
This may seem surprising, but liver inflammation can irritate the diaphragm, which shares nerve pathways with the shoulder area.
The result is referred pain—pain that is felt in a different location from its source.
If someone experiences unexplained right shoulder pain along with digestive issues or fatigue, liver health should be considered.
Another part of the body that may show signs of liver trouble is the skin.
While the skin may not “hurt” in the traditional sense, it can become itchy—a condition known as pruritus.
This happens because when the liver cannot properly process bile, bile salts can build up in the bloodstream and deposit in the skin.
The itching can be intense and persistent, especially at night, and often occurs without a visible rash.
Additionally, the skin and the whites of the eyes may turn yellow, a condition called jaundice.
Jaundice happens when bilirubin, a yellow pigment normally processed by the liver, accumulates in the blood due to impaired liver function.
The stomach and digestive system are also affected.
Since the liver produces bile, which helps break down fats, liver dysfunction can interfere with digestion.
People may experience bloating, nausea, loss of appetite, and discomfort after eating fatty foods.
In more advanced cases, fluid can accumulate in the abdomen—a condition known as ascites.
This can cause visible swelling, tightness, and abdominal pain.
The legs and ankles may also begin to swell.
When liver function declines significantly, it affects the body’s ability to regulate fluid balance and produce proteins like albumin, which helps keep fluid in the bloodstream.
As a result, fluid may leak into surrounding tissues, leading to edema (swelling), particularly in the lower extremities.
The swelling can feel heavy or uncomfortable.
Fatigue is another common symptom, though it is not localized to one body part.
When the liver cannot effectively filter toxins from the blood, these toxins can accumulate and affect overall energy levels.
People often report extreme tiredness, weakness, and difficulty concentrating.
In severe cases, toxin buildup can impact the brain, leading to confusion, memory problems, or mood changes—a condition called hepatic encephalopathy.
The muscles and joints may also feel sore.
Chronic liver disease can lead to inflammation throughout the body.
Additionally, certain liver conditions are associated with autoimmune responses, which can cause joint pain and stiffness.
Muscle cramps are also common, especially at night.
Changes in urine and stool can provide important clues.
Dark urine may indicate elevated bilirubin levels, while pale or clay-colored stools may suggest bile flow obstruction.
Although these symptoms do not involve pain directly, they often accompany abdominal discomfort and signal liver dysfunction.
It is important to understand why liver damage causes symptoms in so many different areas.
The liver acts as a central processing unit for the body.
When it becomes inflamed, scarred (as in cirrhosis), or overwhelmed by fat deposits (as in non-alcoholic fatty liver disease), its ability to regulate metabolism, detoxify blood, and support other organs declines.
This systemic effect explains why symptoms are widespread.
Common causes of liver problems include excessive alcohol consumption, viral hepatitis (such as hepatitis B or C), obesity-related fatty liver disease, certain medications, toxin exposure, and autoimmune disorders.
Early-stage liver disease may produce few or no symptoms, which is why it is sometimes called a “silent” condition.
By the time pain and visible signs appear, significant damage may already have occurred.
The good news is that the liver has remarkable regenerative capacity.
If damage is detected early, lifestyle changes can significantly improve liver health.
Reducing alcohol intake, maintaining a healthy weight, exercising regularly, eating a balanced diet rich in vegetables and lean proteins, and limiting processed foods can all support liver recovery.
Drinking enough water and avoiding unnecessary medications or supplements that strain the liver is also important.

Anyone experiencing persistent upper right abdominal pain, unexplained fatigue, yellowing of the skin, severe itching, swelling, or digestive changes should consult a healthcare professional for proper evaluation.
Blood tests measuring liver enzymes, imaging studies like ultrasound, and other diagnostic tools can determine the extent of liver involvement.
In conclusion, when your liver is “bad,” multiple parts of the body may begin to hurt or show distress.
The upper right abdomen, right shoulder, skin, stomach, legs, and even the brain can be affected.
These symptoms occur because the liver plays such a central role in maintaining overall health.
Recognizing the warning signs early and seeking medical guidance can make a critical difference in preventing long-term complications and preserving liver function.
News in the same category


The Simple Onion Water Ritual: A Natural Way to Refresh Your Scalp and Improve Hair Feel Over Time
What Your Face May Be Telling You About Your Health

A Doctor Explains What “Lightning Bum” Really Is

Painful Underboob Rash? 5 Common Causes You Should Know

Natural Secret to Brighter Eyes: A Drink with Oregano & Polyscias Fruticosa to Support Vision from Within
8 Strange (But Real) Signs Your Body Is Begging for More Vitamin B12 – Don’t Ignore These Red Flags
The Body's Quiet Whispers: 5 Subtle Signs of Cancer You Shouldn't Ignore

The Leaf of Life Plant: A Traditional Herb with Promising Wellness Support That’s Often Overlooked

5 Estrogen-Rich Foods Women Should Eat to Balance Hormones, Achieve Radiant Skin, and Stay Youthful

Can Onions Support Eye Health? A Surprising Kitchen Habit Many Seniors Are Talking About

Boil garlic in milk and drink it all at once: Why you should start doing this
When to Worry About Veins That Appear Out of Nowhere
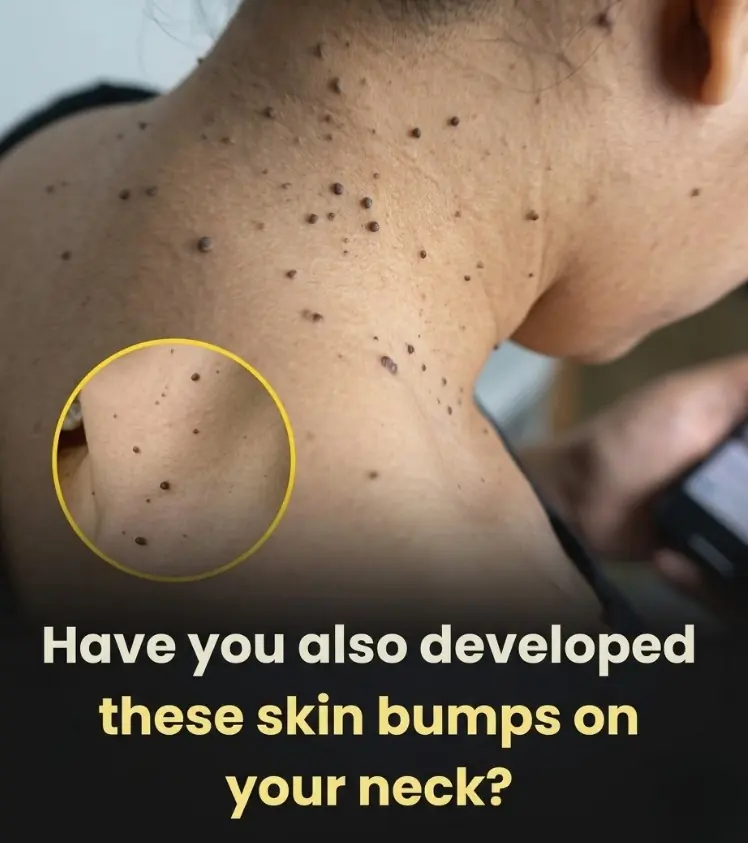
Have you also developed these skin bumps on your neck?
Silent Symptoms of Anemia You Should Never Ignore

Wake Up with Lighter Legs: 6 Bedtime Foods That May Help Improve Circulation

Signs of Aneurysm...
Hip Pain What Your Body Might Be Trying to Tell You
10 Signs Showing Something Is Wrong in Your Body
News Post

These Are the 8 Signs That Indicate You Have Too Much Sugar in Your Body

The Way You Sleep Reveals How Lazy You Are... See more
There are 5 types of feet: each indicating a particular personality type go to the first comment ...👇

WHICH CAR, IF PUT IN REVERSE, WILL SOLVE THIS PROBLEM?

My Sister Stole My Wedding Dress and Walked Down the Aisle With My Fiancé — But I Was Ready for Them

My Foster Son Never Spoke for Years… Until One Day in Court, He Said Something That Stunned Everyone

She Saved 50 Freezing Hells Angels from a Blizzard, What 2,000 Bikers Did Next Made National News

A Hells Angel Went to a Care Home to Donate — Then Found His Long-Lost Mom

I Gave Birth to My Daughter… But Five Years Later, a Doctor Told Me She Isn’t Mine

At 36, I Married the ‘Beggar’ Everyone Mocked—A Year Later, Three Luxury Cars Revealed Who She Really Was

The Simple Onion Water Ritual: A Natural Way to Refresh Your Scalp and Improve Hair Feel Over Time

What Your Face May Be Telling You About Your Health

A Doctor Explains What “Lightning Bum” Really Is
What It Really Means When a Cat Bites You

Painful Underboob Rash? 5 Common Causes You Should Know
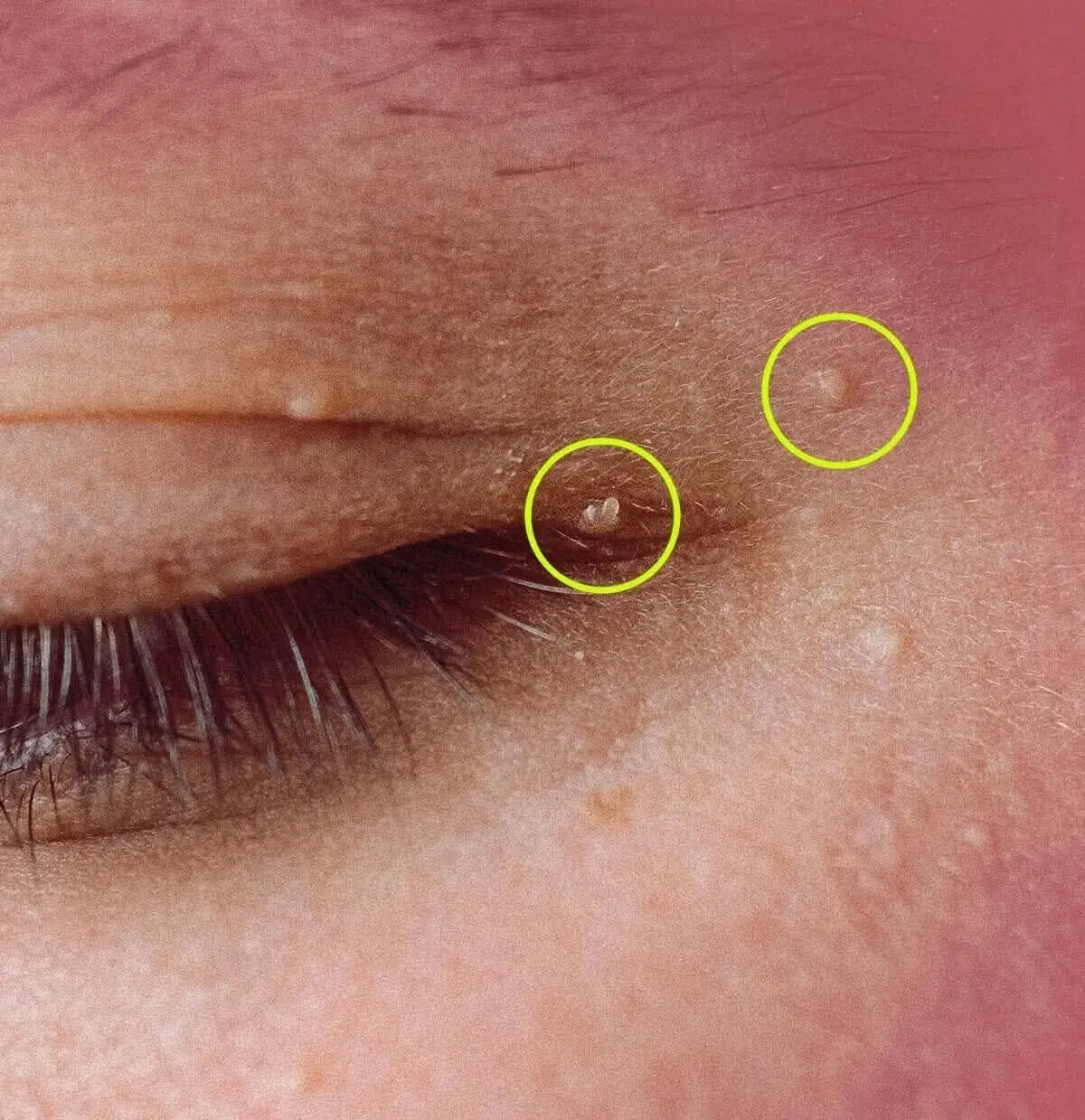
How to Safely Remove Milia

Math problem divides the internet

Natural Secret to Brighter Eyes: A Drink with Oregano & Polyscias Fruticosa to Support Vision from Within
