
My feet feel hot and burning when I lie down at night, even though they’re cold to touch. What’s going on?
The sensation of burning hot feet at night — especially when the skin feels cold to the touch — can be confusing, uncomfortable, and sometimes alarming. Many people describe it as if their feet are on fire internally, yet when they reach down to touch them, the skin feels cool. This strange contradiction is not just about temperature. It often reflects a deeper issue involving nerve signaling, blood circulation, or metabolic health.
Understanding why this happens requires looking beyond the surface. Your body’s nervous system and circulatory system are constantly communicating with each other. When that communication becomes disrupted, sensations can become distorted. Identifying the underlying cause is essential — not just for symptom relief, but for protecting long-term nerve health.
1. Why Your Feet Can Feel Burning Hot Yet Be Cold to the Touch
This phenomenon happens because sensation is controlled by nerves — not by temperature alone. When peripheral nerves become irritated or damaged, they may send incorrect signals to the brain. The brain interprets these faulty signals as heat or burning, even if the actual skin temperature is normal or cold.
At the same time, reduced blood flow can cause the feet to physically feel cold. So while your circulatory system makes your skin cool, your nervous system may be generating a “false alarm” of heat. This mismatch between perception and reality is what creates the paradoxical experience.
Hormonal fluctuations, stress, anxiety, and nighttime circulation changes can further amplify these sensations, making them feel stronger once you lie down to sleep.
2. How Peripheral Neuropathy Triggers Nighttime Burning
One of the most common causes of burning feet is peripheral neuropathy — a condition involving damage to the peripheral nerves.
These nerves are responsible for carrying sensory information from your feet to your brain. When damaged, they can misfire, producing:
-
Burning sensations
-
Tingling or “pins and needles”
-
Numbness
-
Sharp or electric-like pain
Symptoms often worsen at night. Why? Because external distractions decrease, circulation slows slightly during rest, and your brain becomes more aware of internal sensations.
Neuropathy has many causes, including diabetes, infections, autoimmune disorders, toxin exposure, and chronic inflammation. In some cases, it develops gradually and may go unnoticed until nighttime symptoms become disruptive.
3. Circulation Problems and Confused Temperature Signals
Poor circulation can also play a significant role. Conditions such as peripheral artery disease (PAD) reduce blood flow to the extremities, making feet feel cold. However, insufficient oxygen supply can irritate surrounding nerves, triggering burning sensations.
Venous insufficiency — when veins struggle to return blood to the heart — can cause blood pooling in the lower legs. This can create pressure, heaviness, and burning discomfort, particularly when lying down.
Gravity, prolonged sitting, dehydration, and inactivity can worsen circulation issues, intensifying symptoms at night.
4. Diabetes, Prediabetes, and Metabolic Syndrome
High blood sugar is one of the most common causes of nerve damage worldwide. Over time, elevated glucose levels damage small blood vessels that supply nerves, leading to diabetic neuropathy.
Even prediabetes can begin affecting nerve fibers before a formal diabetes diagnosis. Burning feet at night may be an early warning sign.
Metabolic syndrome — a cluster of conditions including insulin resistance, abdominal obesity, high blood pressure, and abnormal cholesterol — increases inflammation and impairs circulation. Together, these factors create the perfect environment for nerve irritation and temperature misinterpretation.
Early detection is crucial because nerve damage becomes harder to reverse once advanced.
5. Vitamin Deficiencies and Alcohol Use
Certain nutrients are essential for nerve repair and function, especially:
-
Vitamin B12
-
Vitamin B6
-
Folate
-
Vitamin B1 (thiamine)
Deficiencies can lead to nerve degeneration and abnormal sensations. Long-term alcohol use not only directly damages nerve tissue but also interferes with nutrient absorption, compounding the problem.
Poor diet, restrictive eating patterns, gastrointestinal disorders, and certain medications can all contribute to vitamin deficiencies that quietly affect nerve health.
6. Medication Side Effects and Environmental Toxins
Some medications can unintentionally irritate peripheral nerves. Chemotherapy drugs are well-known for causing neuropathy, but certain antibiotics, antivirals, and heart medications may also have nerve-related side effects.
Exposure to heavy metals such as lead, mercury, or arsenic can damage nerve fibers. Occupational exposure, contaminated water, or long-term environmental contact may contribute.
Sometimes, burning feet are not caused by disease itself — but by what the body has been exposed to over time.
7. Back Problems and Nerve Compression
The problem may not originate in your feet at all.
Conditions such as herniated discs, spinal stenosis, or degenerative disc disease can compress nerves in the lower back. When these nerves are irritated, pain and burning sensations can travel down the legs into the feet.
Sciatica, involving compression of the sciatic nerve, may cause radiating pain, tingling, or burning that reaches the foot. In these cases, the skin temperature remains normal — but the nerve pathway is inflamed.
8. Simple At-Home Observations
While not a replacement for medical diagnosis, some simple checks may provide clues:
-
Color changes: Pale or bluish feet may indicate poor circulation; redness could suggest inflammation.
-
Sensation testing: Lightly touch your feet with cotton or a soft cloth to check for reduced sensation.
-
Symmetry: If both feet are equally affected, neuropathy is more likely. If only one foot is affected, nerve compression may be involved.
-
Temperature comparison: Compare foot temperature to your calves or hands.
If symptoms are persistent, worsening, or accompanied by weakness, medical evaluation is important.
9. When to See a Doctor
You should seek medical attention if you experience:
-
Persistent burning lasting weeks
-
Numbness or muscle weakness
-
Balance problems
-
Unexplained wounds on your feet
-
Symptoms worsening over time
Doctors may recommend:
-
Blood tests (glucose, vitamin levels, thyroid function)
-
Nerve conduction studies
-
Electromyography (EMG)
-
Imaging such as MRI for spinal evaluation
Early intervention can prevent progression and protect long-term mobility.
10. Nighttime Relief Strategies
To soothe burning, cold-feeling feet at night:
-
Elevate your legs to improve circulation
-
Use a cool compress or fan for temporary relief
-
Try topical creams with capsaicin or lidocaine
-
Perform gentle stretching before bed
-
Massage feet to stimulate blood flow
-
Wear breathable socks (avoid overheating)
Stress reduction techniques such as deep breathing or relaxation exercises may also help, as stress can amplify nerve sensitivity.
11. Long-Term Nerve Protection
Protecting your nerves requires addressing root causes.
-
Keep blood sugar stable
-
Maintain a balanced diet rich in B vitamins and antioxidants
-
Exercise regularly to improve circulation
-
Stay hydrated
-
Limit alcohol
-
Avoid smoking
-
Monitor cholesterol and blood pressure
Regular check-ups help detect changes early. Nerve health is closely tied to metabolic and vascular health — taking care of one supports the other.
Final Thoughts
Burning feet at night, especially when cold to the touch, are not “just in your head.” They are often signals from your nervous or circulatory system asking for attention. While the sensation may seem minor at first, it can be an early warning of deeper imbalances.
Listening to these signals — and responding proactively — can prevent long-term complications and restore comfort, sleep quality, and overall well-being.
News in the same category


Experts Warn Avoid These 4 Foods If You Want to Live Longer

The #1 Kitchen Mistake That’s Making Your Family Sick (And Ruining Your Food)

🏠 8 Household Items That Could Be Affecting Your Health (And How to Check Them Safely at Home)

Subtle Signs You’re Not Drinking Enough Water

Beets The Superfood That Actually Lives Up to the Hype

I have absolutely no idea! Let's see why.
A Traditional Natural Compress for Joint and Tendon Comfort

The Surprising Health Benefits of Coffee

Simple Ways to Slow Wrinkles and Keep Your Skin Glowing
Did you know that...

Here’s what the letter ‘M’ and the crescent moon on the palm of your hand truly signify

The Easy Trick to Make Stainless Steel Sparkle

Why Some People Put Water Bottles Outside Their Homes

🥦 3 Vegetables That Support Cancer Prevention — Backed by Science

Signs and Symptoms of Oral Cancer

The Best Time To Drink Pomegranate Juice for Better Blood Pressure and Muscle Recovery
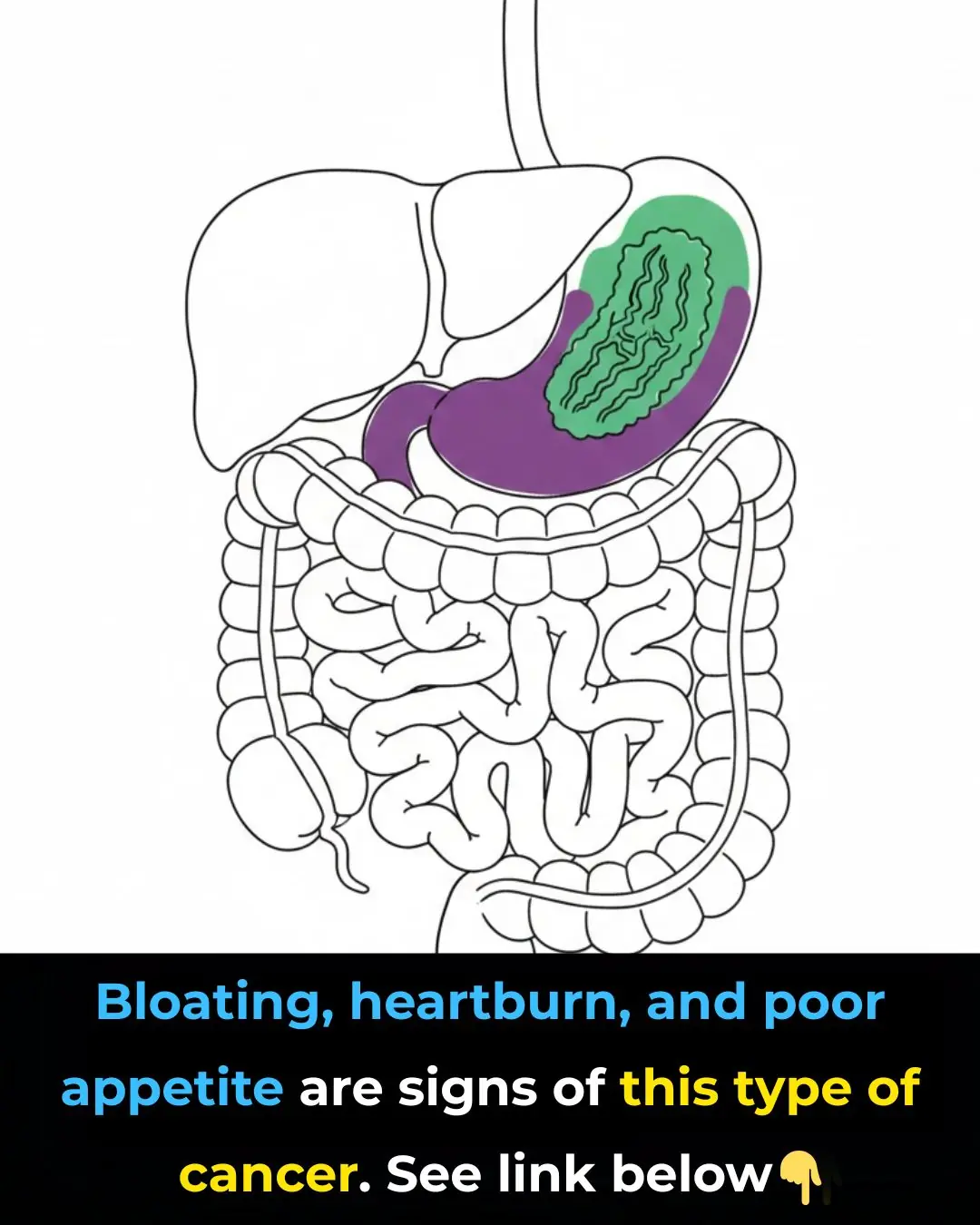
What Is Stomach Cancer?
What Is the Adam’s Apple
News Post

Reducing Prostate Discomfort Naturally with a Tomato and Garlic Drink

Never Throw Away the Avocado Seed Again — Here’s Why

Guava Leaves Benefits: The Underrated Natural Remedy You Shouldn’t Ignore 🍃💪

Herbal Tea for Swollen Legs: Natural Diuretic & Anti-Inflammatory Recipe, How to Use It, and Precautions
Avocado Seed Benefits: The Overlooked Natural Remedy for Joint and Back Pain
How Garlic and Lemon Can Gently Support Your Eye Comfort and Vision Wellness

Was He Really Jesus?

Pumpkin Seeds

The Overlooked Tree With Powerful Health Benefits

Discover How Incorporating Fresh Parsley into Your Daily Routine Can Support Knee Joint Comfort and Mobility Naturally

Woman reveals 3 overlooked symptoms before her stage 4 cancer diagnosis at 28

The Funeral Secret
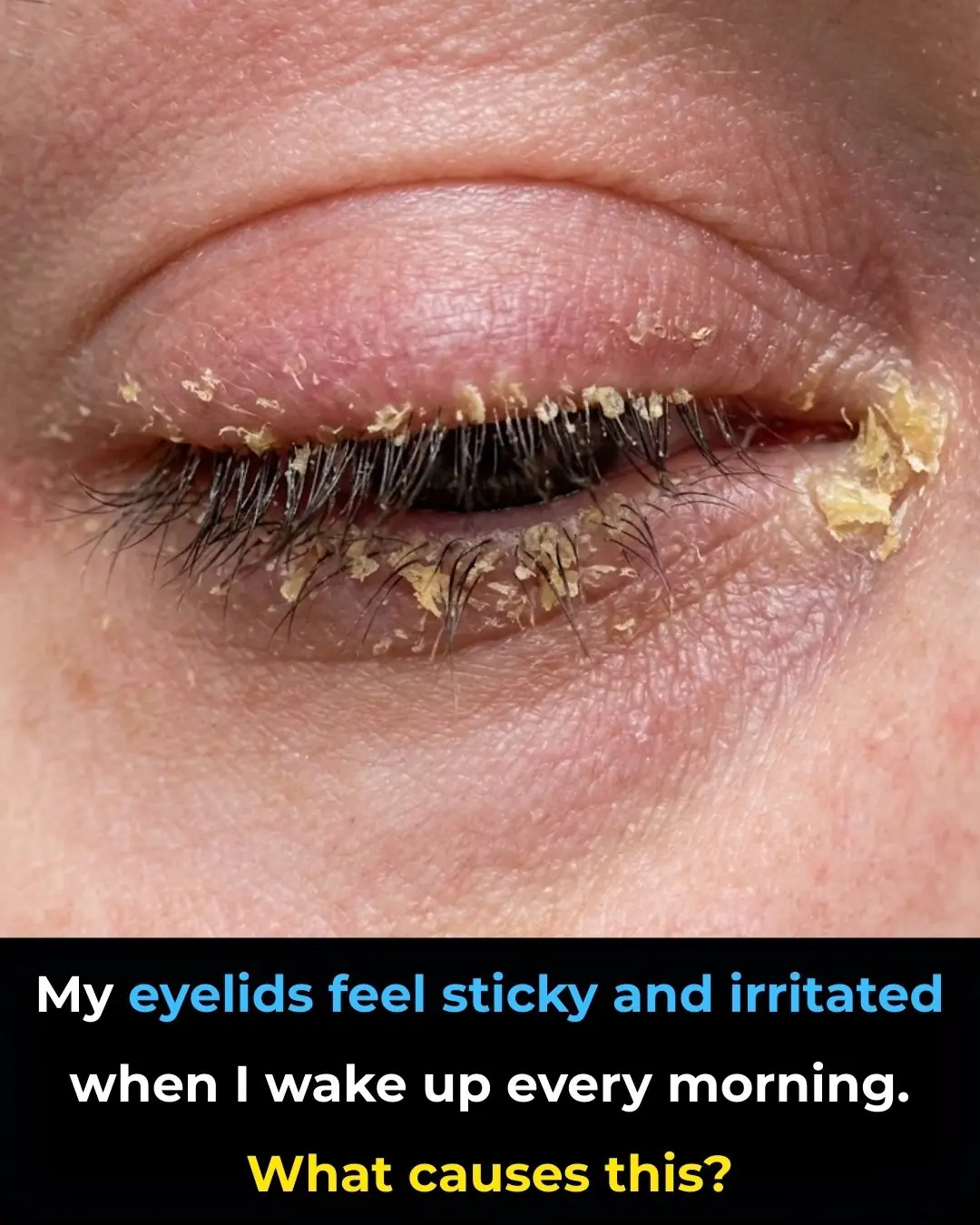
My eyelids feel sticky and irritated when I wake up every morning. What causes this?

One Spoon a Day for Stronger Vision – A Simple Daily Habit to Support Eye Comfort

A Gentle Herbal Infusion to Support Blood Sugar, Cholesterol & Circulation Naturally

Mother’s Silent Sacrifice
Home Remedies for Varicose Veins with Onion, Garlic, and Apple Cider Vinegar

The Watch That Changed Everything
