Everything You Need To Know About Nail Pitting
:max_bytes(150000):strip_icc():format(webp)/Health-GettyImages-1645966065-2bece96c95c349dbbcea8f50dfb75216.jpg)
Nail pitting refers to the appearance of small dents, depressions, or tiny holes in the surface of the nails. These indentations develop when the nail matrix — the area responsible for producing new nail cells — becomes inflamed or disrupted. Nail pitting is most commonly associated with autoimmune conditions, especially psoriatic arthritis (PsA), but it can occur with several other disorders as well.
Treatment depends largely on the underlying cause. In many cases, controlling the primary condition helps reduce nail symptoms and prevent flare-ups.
What Causes Nail Pitting?
Your nails are formed in a specialized layer of cells called the nail matrix. Within this matrix, keratinocytes produce keratin, the protein that hardens and shapes the nail plate. When inflammation, injury, or immune dysfunction interferes with this process, abnormal keratin formation occurs — leading to visible pits in the growing nail.
Nail pitting is usually a symptom rather than a standalone condition.
Common Conditions Linked to Nail Pitting
Psoriasis
Psoriasis is an autoimmune disorder that causes rapid skin cell turnover. When the immune system attacks cells in the nail matrix, immature keratinocytes are formed. As the nail grows outward, these defective areas appear as pits.
Nail pitting is especially common in people who develop Psoriatic arthritis, an inflammatory condition affecting both joints and skin. In fact, nail changes may be one of the earliest signs of PsA.
Alopecia areata
Alopecia areata occurs when the immune system attacks hair follicles, typically causing patchy hair loss on the scalp or face. However, it can also affect the nails. Nail pitting associated with this condition may be shallow but widespread.
Dyshidrotic eczema
This condition causes small, itchy blisters on the hands and feet, often triggered by stress, irritants, or allergens. Chronic inflammation from dyshidrotic eczema may eventually disrupt nail growth, resulting in pitting.
Reactive arthritis
Reactive arthritis develops after certain gastrointestinal or genitourinary infections. The immune response triggered by infection may affect joints, eyes, skin — and occasionally the nails. Nail changes are less common but possible.
Sarcoidosis
Sarcoidosis involves the formation of inflammatory cell clusters (granulomas) in organs such as the lungs. Nail involvement is rare, but when it occurs, it often signals systemic disease.
How to Recognize Nail Pitting
Nail pitting appears as:
-
Small, round depressions in the nail surface
-
Shallow or deep dents
-
Evenly spaced or randomly distributed pits
-
One nail or multiple nails affected
In psoriasis-related nail pitting, pits are often uniform in size and depth. Some individuals may also develop onycholysis, a condition in which the nail plate separates from the nail bed. Having 10 or more pits in one nail — or more than 50 across all nails — strongly suggests psoriasis.
Other associated nail symptoms may include:
-
Brittle or crumbly nails
-
Discoloration
-
Thickening
-
Rough texture
-
Cracking
Symptoms can vary depending on the underlying disorder.
How Is Nail Pitting Diagnosed?
A healthcare provider — often a dermatologist — can usually identify nail pitting through physical examination. To determine the underlying cause, additional tests may be recommended, including:
-
Blood tests to detect inflammation or autoimmune markers
-
Imaging studies if systemic disease (such as sarcoidosis) is suspected
-
Nail biopsy to examine matrix tissue
-
Nail clippings to rule out fungal infections
Accurate diagnosis is important because treatment targets the root cause, not just the cosmetic appearance.
Treatment Options
Improvement takes time. Nails grow slowly, so visible results may take six months or longer.
Topical Medications
Corticosteroid creams or ointments may reduce inflammation in mild cases.
-
Calcipotriol (vitamin D derivative) can help reduce abnormal nail buildup.
-
Tazarotene (a vitamin A derivative) may improve nail texture and pitting.
Intralesional Steroid Injections
In moderate cases, a doctor may inject corticosteroids directly into or near the nail matrix every 4–6 weeks. This approach targets inflammation more directly.
Systemic Medications
For severe or widespread disease, systemic treatments may be necessary. These include:
-
Biologic medications
-
Disease-modifying antirheumatic drugs (DMARDs), such as methotrexate
These therapies regulate immune activity and are often used in psoriatic arthritis or severe psoriasis.
Tips to Help Prevent Nail Pitting Flares
While you may not be able to prevent the underlying autoimmune condition, you can reduce flare risk by:
-
Managing stress
-
Avoiding nail trauma or picking
-
Keeping nails trimmed and clean
-
Moisturizing regularly
-
Following prescribed treatment plans consistently
-
Treating skin or joint symptoms early
Protective gloves may also help reduce irritation if you frequently expose your hands to water or chemicals.
Final Takeaway
Nail pitting is more than a cosmetic concern — it can be a visible clue that your immune system is active beneath the surface. Because it is often linked to autoimmune conditions, early evaluation and treatment are important.
If you notice persistent dents, nail separation, or other unusual nail changes, consult a healthcare professional. Identifying and treating the underlying condition can not only improve the appearance of your nails but also protect your overall health.
News in the same category


How To Identify Skin Tags and When To Remove Them
14 Visible Signs of Cancer Most Women Ignore

Reducing Prostate Discomfort Naturally with a Tomato and Garlic Drink

Never Throw Away the Avocado Seed Again — Here’s Why

Guava Leaves Benefits: The Underrated Natural Remedy You Shouldn’t Ignore 🍃💪

Herbal Tea for Swollen Legs: Natural Diuretic & Anti-Inflammatory Recipe, How to Use It, and Precautions
Avocado Seed Benefits: The Overlooked Natural Remedy for Joint and Back Pain
How Garlic and Lemon Can Gently Support Your Eye Comfort and Vision Wellness

The Overlooked Tree With Powerful Health Benefits

Discover How Incorporating Fresh Parsley into Your Daily Routine Can Support Knee Joint Comfort and Mobility Naturally

Woman reveals 3 overlooked symptoms before her stage 4 cancer diagnosis at 28
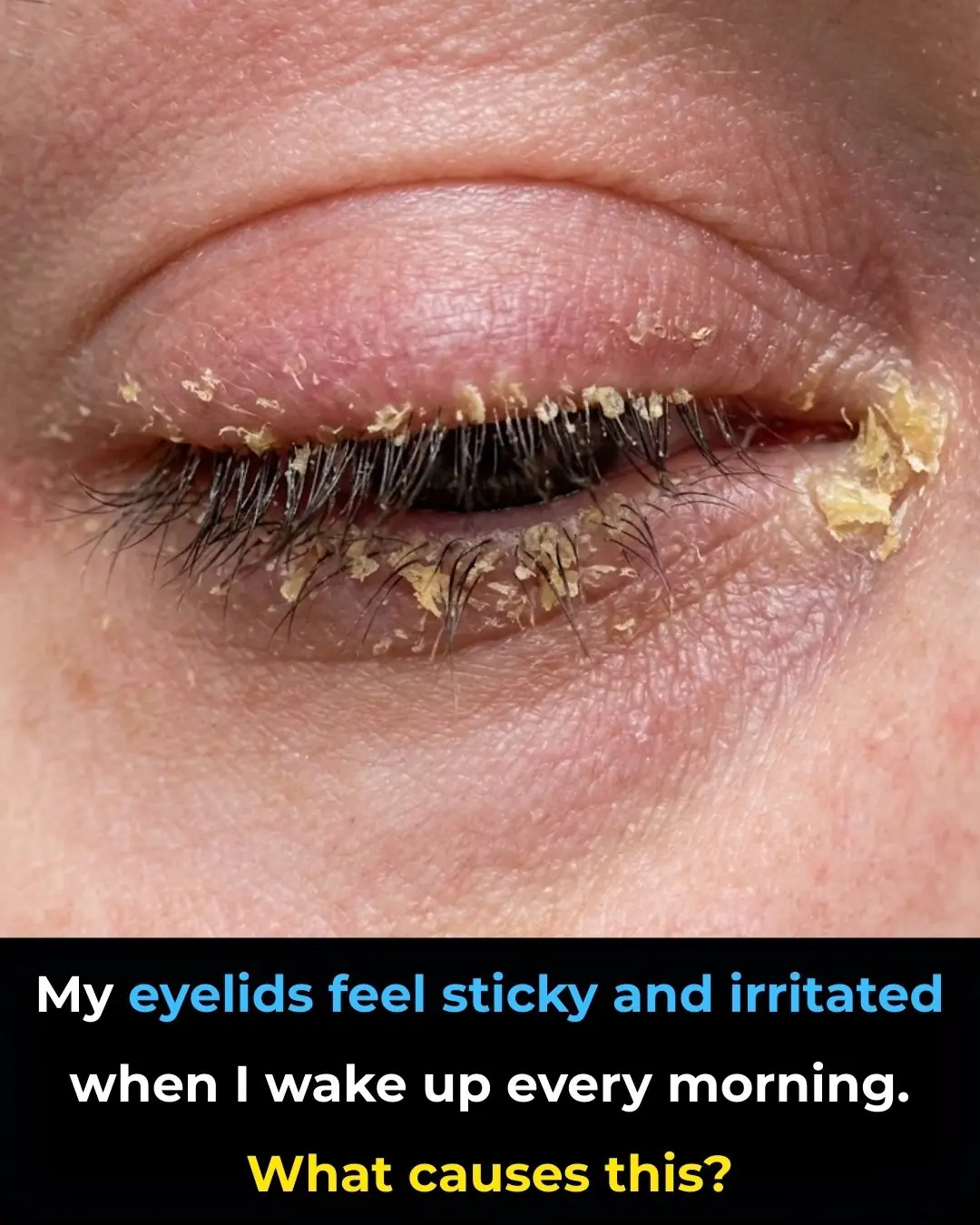
My eyelids feel sticky and irritated when I wake up every morning. What causes this?

One Spoon a Day for Stronger Vision – A Simple Daily Habit to Support Eye Comfort

A Gentle Herbal Infusion to Support Blood Sugar, Cholesterol & Circulation Naturally
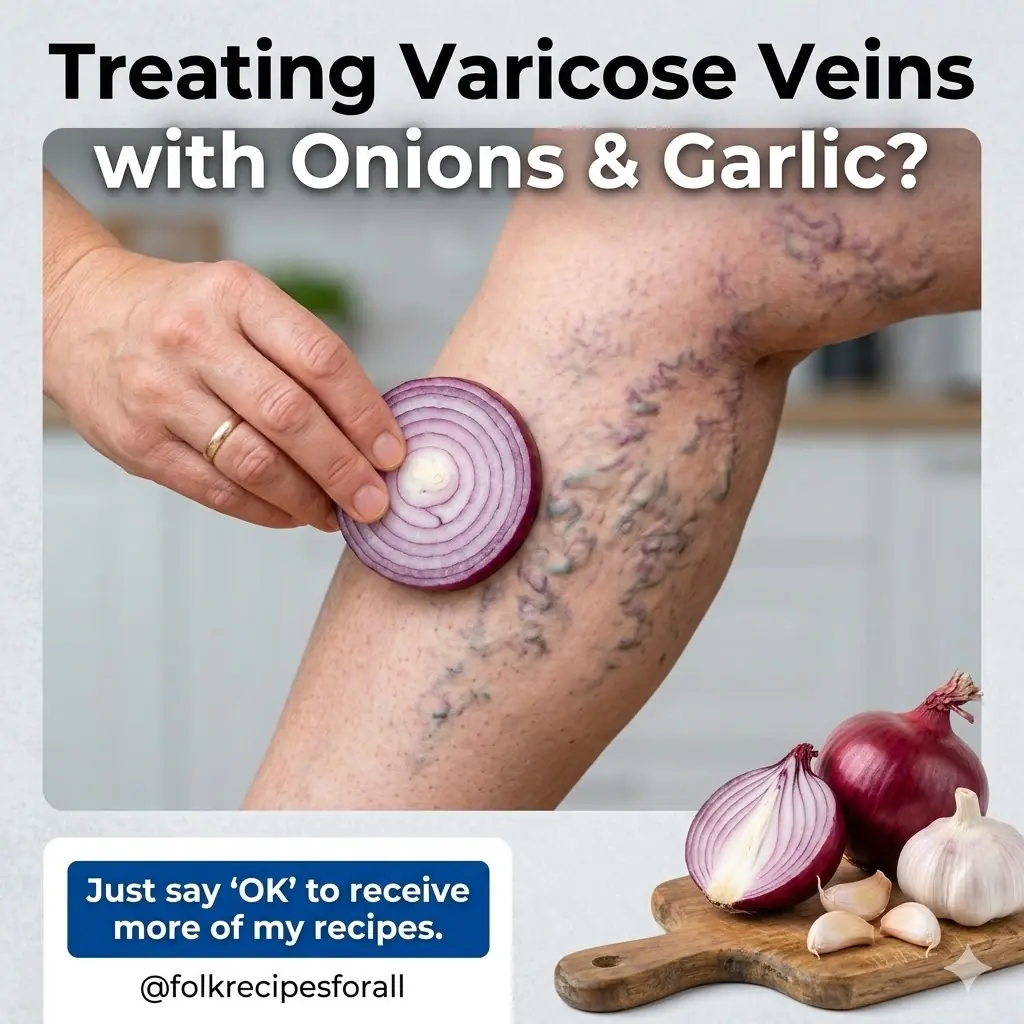
Home Remedies for Varicose Veins with Onion, Garlic, and Apple Cider Vinegar
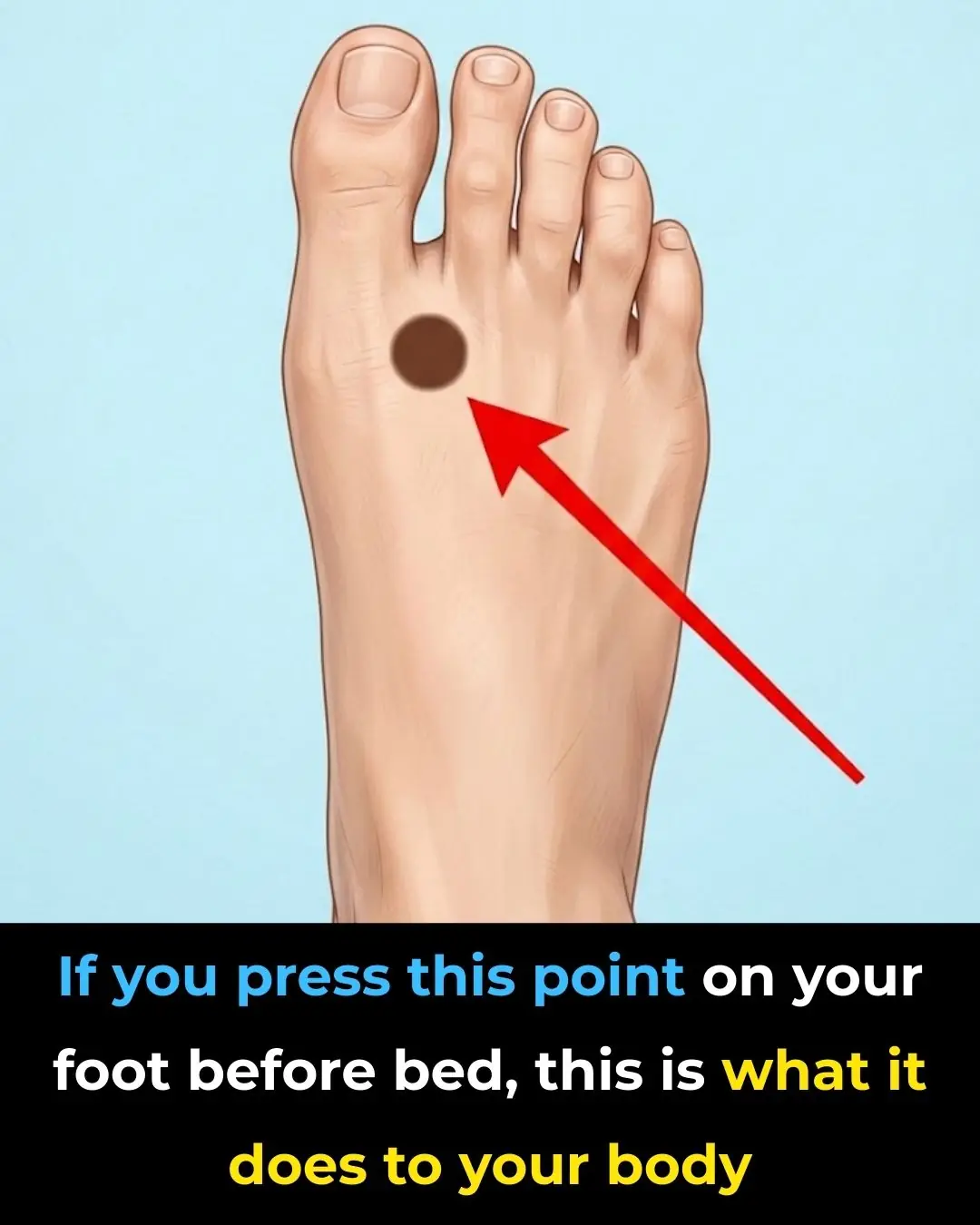
Press This Point on Your Feet Before Bed
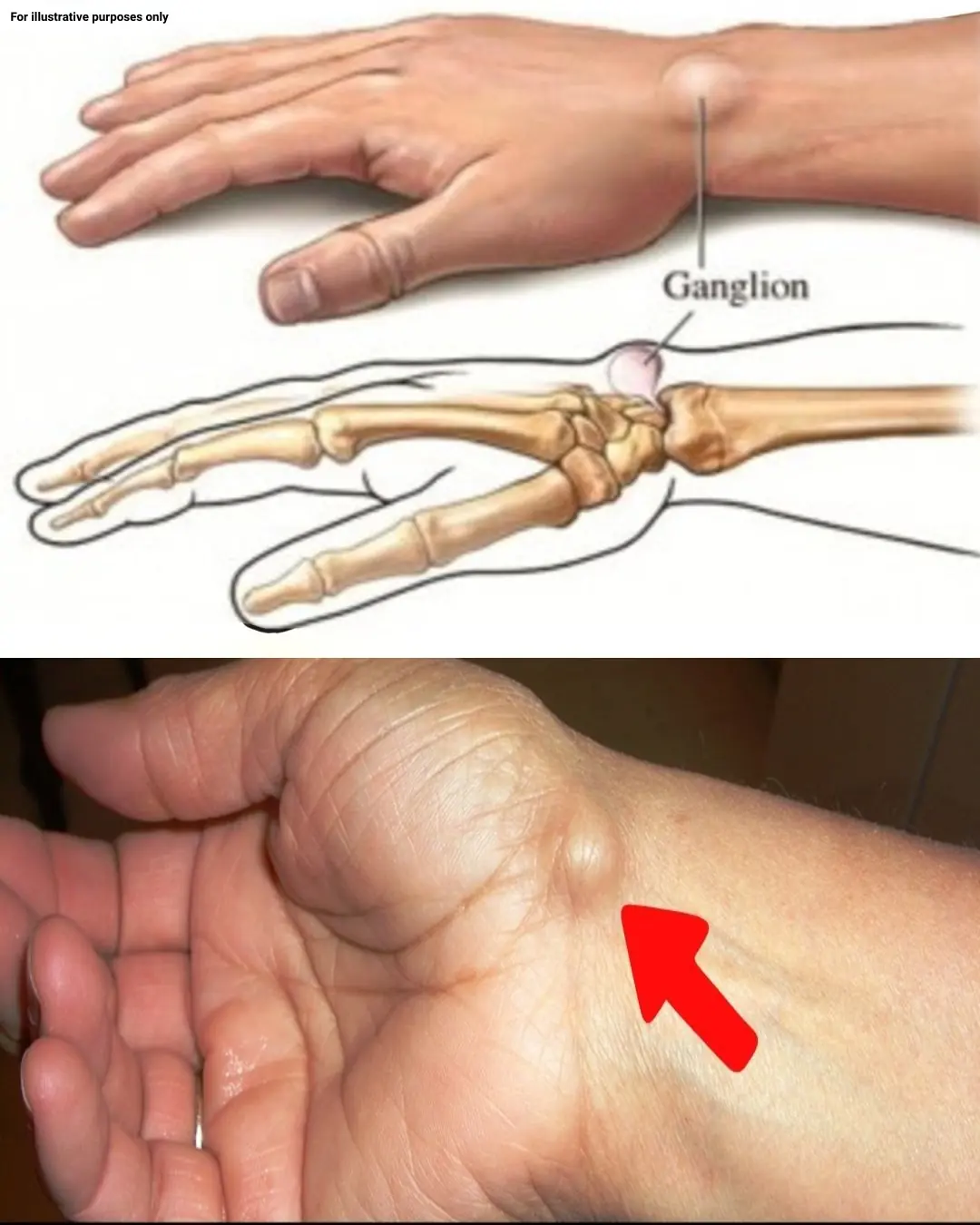
Noticing a Lump on Your Hand
More Than a Moment: Understanding the Layers of Intimacy
News Post

🧠 8 Strange (But Real) Signs Your Body Is Begging for More Vitamin B12 – Don’t Ignore These Red Flags

How To Identify Skin Tags and When To Remove Them

14 Visible Signs of Cancer Most Women Ignore

Reducing Prostate Discomfort Naturally with a Tomato and Garlic Drink

Never Throw Away the Avocado Seed Again — Here’s Why

Guava Leaves Benefits: The Underrated Natural Remedy You Shouldn’t Ignore 🍃💪

Herbal Tea for Swollen Legs: Natural Diuretic & Anti-Inflammatory Recipe, How to Use It, and Precautions

Avocado Seed Benefits: The Overlooked Natural Remedy for Joint and Back Pain

How Garlic and Lemon Can Gently Support Your Eye Comfort and Vision Wellness

Was He Really Jesus?

Pumpkin Seeds

The Overlooked Tree With Powerful Health Benefits

Discover How Incorporating Fresh Parsley into Your Daily Routine Can Support Knee Joint Comfort and Mobility Naturally

Woman reveals 3 overlooked symptoms before her stage 4 cancer diagnosis at 28

The Funeral Secret

My eyelids feel sticky and irritated when I wake up every morning. What causes this?

My feet feel hot and burning when I lie down at night, even though they’re cold to touch. What’s going on?

One Spoon a Day for Stronger Vision – A Simple Daily Habit to Support Eye Comfort
