
Gynecologist Refuses to Treat Trans Woman, Sparking Backlash Over Refused Care

Jessica Yaniv, a transgender woman from Canada, has once again found herself at the center of a heated debate on transgender rights and medical ethics. Yaniv recently filed a formal complaint after she was allegedly denied care by a gynecologist due to her transgender status. The controversy comes in the wake of previous cases Yaniv brought against beauty salons that refused to perform waxing services on her, sparking national and international attention.
This latest incident has reignited discussions around healthcare access for transgender individuals, doctor responsibilities, medical qualifications, and the evolving definition of patient rights in the healthcare system.
“We Don’t Serve Transgender Patients”
According to Yaniv, the gynecologist’s office told her directly, “We don’t serve transgender patients.” She took to social media shortly after, expressing her feelings of disbelief, frustration, and hurt.
“I was shocked… confused… and hurt,” she wrote, describing the emotional toll of being turned away by a medical professional. In a post that tagged the College of Physicians and Surgeons of British Columbia, Yaniv questioned whether such a refusal was even legal under provincial healthcare standards.
“Are they allowed to do that, legally? Isn’t that against the college practices?” she tweeted.
In response, Yaniv claimed that she received confirmation from the College that refusing treatment to transgender patients constitutes discrimination. However, the College later issued a statement clarifying that its staff do not offer legal or ethical opinions over the phone. Instead, callers are directed to consult published professional standards and decide for themselves whether to proceed with a formal complaint.
A Pattern of Legal Action
This is not Yaniv’s first confrontation with service providers over transgender rights. In 2019, she lodged several complaints with the British Columbia Human Rights Tribunal against Vancouver-area aestheticians who refused to provide Brazilian waxing services on her male genitalia. The case drew significant public backlash and media scrutiny.
Yaniv sought up to $15,000 in damages from each business, some of which ended up closing permanently due to legal costs and lost business. Ultimately, the tribunal dismissed the complaints, ruling that Yaniv’s motives appeared to be rooted more in financial gain and personal grievance than in a sincere effort to address discrimination. The tribunal concluded that her actions were "improper" and "targeted small businesses."
When Medical Professionals Refuse Care
The gynecologist involved in the current complaint has not issued any public comment. However, similar cases have occurred globally, underscoring the complexities of transgender healthcare.
In France, a doctor who initially declined to treat a transgender woman stated: “I told her I wasn’t competent, but I can guide her to someone who is.” Although the doctor cited professional boundaries, he later made controversial remarks about treating “real women” — comments for which he publicly apologized.
Medical professionals often cite anatomical and surgical differences as justification for deferring care. One gynecologist explained, “Just because it’s a cavity doesn’t mean it’s a classic vagina,” emphasizing that post-operative neo-vaginas differ significantly from natal female anatomy and often require specialized medical understanding.
A senior gynecology expert further clarified: “There is no standard medical recommendation for a transgender woman to undergo regular gynecological exams unless she has complications from surgery, as she does not have a cervix or uterus.”
Transgender Healthcare Education Still Catching Up
Historically, most medical schools lacked adequate training on transgender health issues. Only in recent years have institutions begun to integrate these topics into their curricula. Today, more universities and medical boards are developing dedicated training programs to help doctors offer respectful and informed care to transgender patients.
Despite these advancements, many practicing doctors still feel unprepared to treat trans individuals, leading to uncomfortable encounters or outright refusals of care — especially when procedures fall outside their perceived scope of practice.
Drawing Ethical Boundaries in Medical Care
Yaniv’s case reflects a broader ethical dilemma: how can healthcare systems protect the rights of transgender patients while also respecting a physician’s right to refer patients when they're not trained or comfortable with certain procedures?
In Canada, legal protections against discrimination based on gender identity vary from province to province. Generally, the law differentiates between declining treatment because of a patient’s identity (which is prohibited) and turning down a procedure due to a lack of relevant medical training (which may be permitted, especially if accompanied by a proper referral).
A patient rights advocate emphasized: “LGBTQ people aren’t asking for different care — just competent care. Medical care doesn’t become ‘special’ just because the patient is transgender.”
However, the reality remains complicated. Many transgender patients report being dismissed, mistreated, or left without care — not due to a lack of technical skill, but due to personal bias or systemic oversight.
The Real-World Risks of Denied Care
These situations aren’t just about emotional harm. Delays or denials in treatment can lead to severe, sometimes fatal, consequences. One documented case involved a transgender man who spent nearly a year searching for a gynecologist willing to see him. By the time he found one, he was diagnosed with advanced ovarian cancer.
“I had every resource, every connection — and I still almost died because nobody would treat me,” he said. His experience echoes a larger trend. A recent survey revealed that nearly 25% of transgender individuals had avoided seeking medical care due to fear of discrimination. Among those who did visit healthcare providers, nearly half reported negative or even hostile experiences.
Building a More Inclusive Medical System
Medical experts say that the path forward lies not in forcing doctors into unfamiliar territory, but in setting clearer expectations around when referral is appropriate — and when refusal becomes discrimination.
A director of a transgender healthcare center explained: “Saying ‘I don’t know how to help you’ isn’t inherently wrong — but saying ‘I won’t help you because you’re trans’ is.” The key, she noted, is accountability and education.
A healthcare educator added: “We need to stop treating transgender patients like outliers. Every medical student should graduate with basic competency in transgender health — just like they would with any other population group.”
As healthcare needs continue to evolve, especially with transgender populations becoming more visible and vocal, systemic reforms become increasingly urgent. In one European country, the number of individuals diagnosed with gender dysphoria in 2020 was ten times higher than in 2013, showing that this is not a fringe issue — it is a growing demand in mainstream healthcare.
The Bigger Picture
Yaniv’s complaint is still under review. The College of Physicians and Surgeons of British Columbia has declined to comment on any ongoing investigations, citing confidentiality and legal constraints.
But the questions her case raises remain unresolved: What does inclusive care really mean? When does professional limitation cross the line into discrimination? And how can medical systems evolve to meet the needs of all patients — regardless of gender identity?
As the world pays closer attention to transgender healthcare access, the stakes grow higher. The ultimate goal, experts agree, is to build a healthcare system where dignity, respect, and appropriate care are not conditional — but guaranteed.
News in the same category


The US deploys an aircraft carrier to participate in the blockade of Iranian ports

Iran Strikes Back: Drone Attacks Target US Vessels After Cargo Ship Seizure

Iran Vows Retaliation After US Seizes Cargo Ship in Gulf of Oman

Iran Accuses the US of “Piracy” After Cargo Ship Seizure Amid Rising Tensions

Iran is ready to 'play a new card on the battlefield'
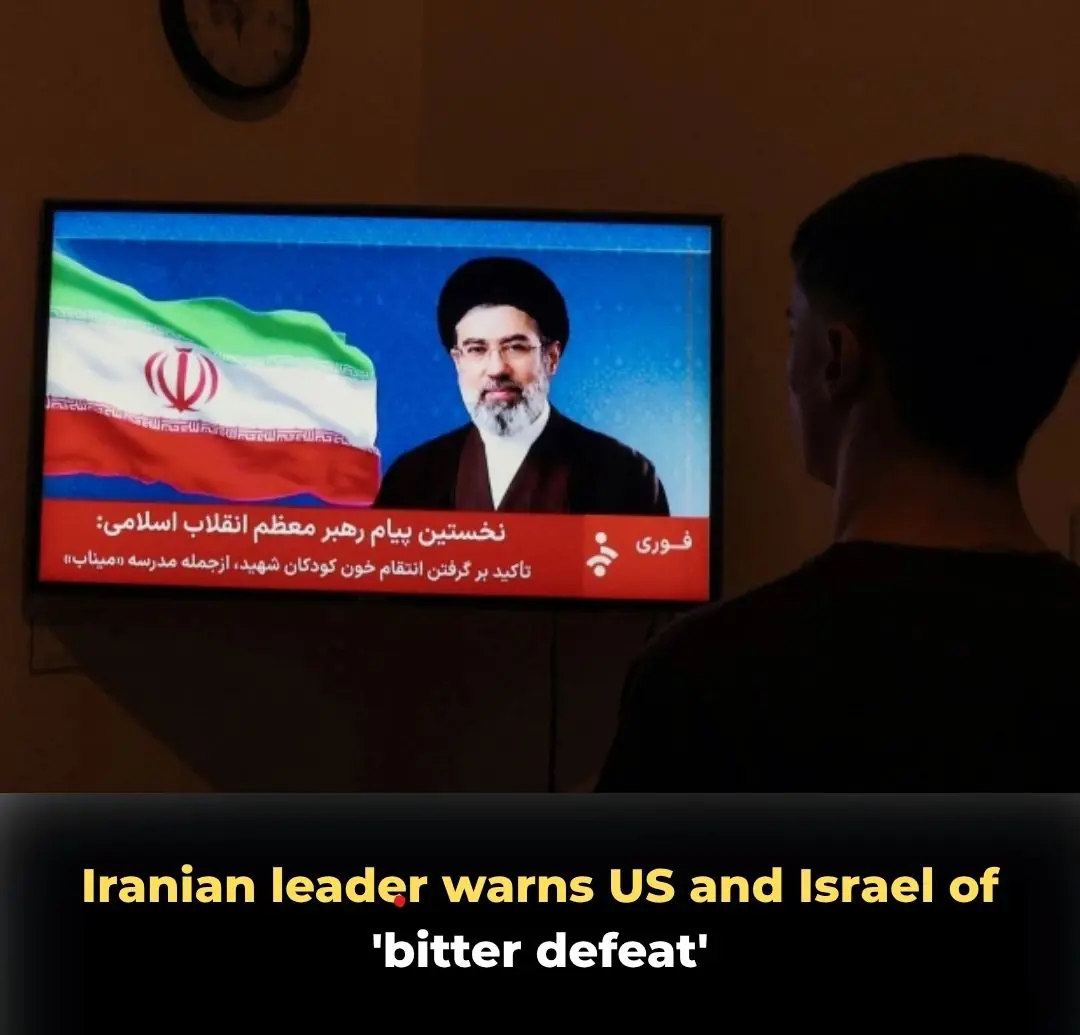
Iran’s Supreme Leader Warns US and Israel of "Bitter Defeat" Amid Rising Maritime Tensions

Iran Claims Drone Attack on US Warships Following Seizure of Iranian Vessel

Iran’s Strategic Shift: Deploying New "Tactical Cards" on the Regional Battlefield

Gasoline tank theft is rampant in the US as fuel prices rise

Trump Issues New Threats Against Iran: "Every Bridge and Power Plant" at Risk

Iran Launches UAV Strikes on U.S. Warships in Sea of Oman Following Ship Seizure

Iran claims to have launched a drone attack on a US warship

US warships fire artillery and seize Iranian cargo ships
Iranian leader warns US and Israel of 'bitter defeat'

Iranian boats attack oil tankers in the Strait of Hormuz

Iran reimposes restrictions on the Strait of Hormuz
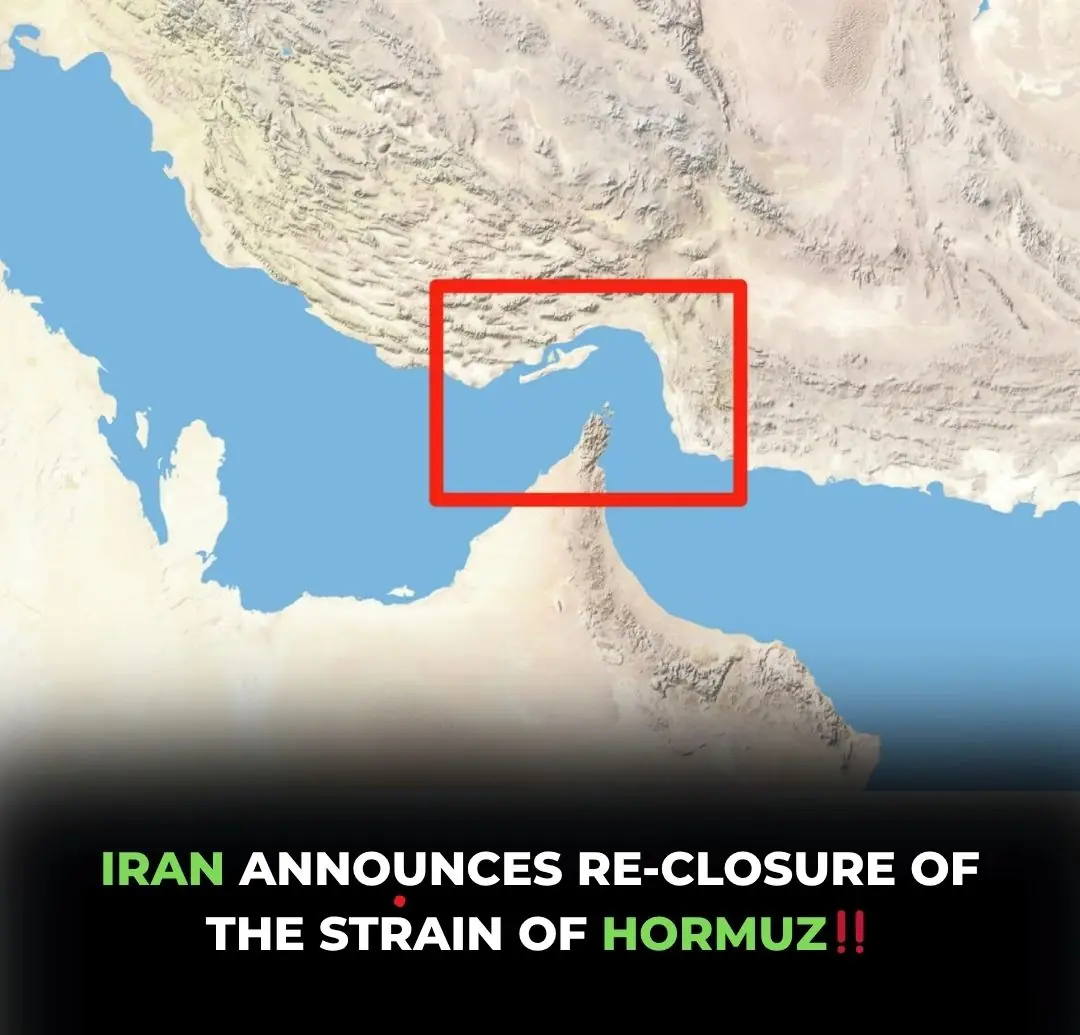
BREAKING: Iran Threatens to Close Strait of Hormuz - Global Oil Shock Looming?... Read more

Ships hesitate to pass through the Strait of Hormuz after announcement of its opening

The US and Iran issue conflicting statements about their enriched uranium stockpiles
News Post

From Thin, Lifeless Hair to Fuller, Healthier Strands: What Actually Works (Expert Perspective)

PART 2: “Why Ellie Knew”

The Pendant That Revealed a Sixteen-Year Secret

PART 2: “Who He Really Was”
Signs of Arthritis You Shouldn’t Ignore

Do They Sense You at the Cemetery
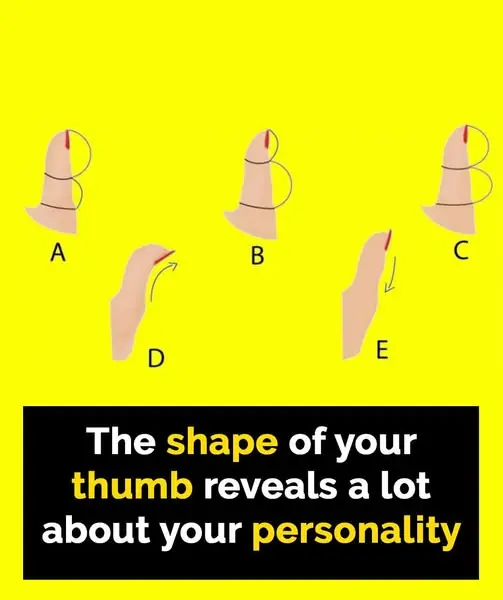
The Secrets Your Thumb Shape Reveals

The Iranian ship may have been carrying 'dual-use cargo' when it was seized by the US

If You See a Turtle or a Camel First — What It Reveals About How Your Brain Works

✨ Why DIY Hair Tonics Alone Are NOT Enough (Expert POV)

The US deploys an aircraft carrier to participate in the blockade of Iranian ports

Part 2: The little girl didn’t understand the sentence.

Part 2: The little girl didn’t understand the sentence

Iran Strikes Back: Drone Attacks Target US Vessels After Cargo Ship Seizure

Iran Vows Retaliation After US Seizes Cargo Ship in Gulf of Oman

Iran Accuses the US of “Piracy” After Cargo Ship Seizure Amid Rising Tensions

PART 2: “Why Her Father Was Crying”

PART 2: “Why They Called Her Princess”

Part 2 : Then—breathing. Heavy. Unstable.
